Mammographic Breast Tissue Density (for Doctors)
Mammographic Breast Tissue Density (for Doctors)
Mammographic Breast Tissue Density and Digital Breast Tomosynthesis
At Sydney Breast Clinic, we always report the density of the breast tissue on the mammogram. What does this mean to you, the referring doctor, and what does it mean for your patient?
Increased mammographic density is a major independent risk factor for the development of breast cancer
On a mammogram the breast is made up of dark areas (fat) and light areas (glandular and fibrous tissue).
The Royal Australian and New Zealand College of Radiologists and Cancer Australia recommend that mammographic breast tissue density be routinely reported, and categorised in quartiles of area percentage density1:
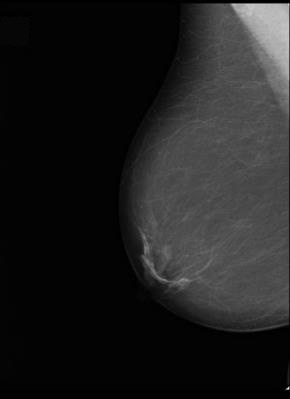
Category A
<25% fibroglandular
(mainly fat)
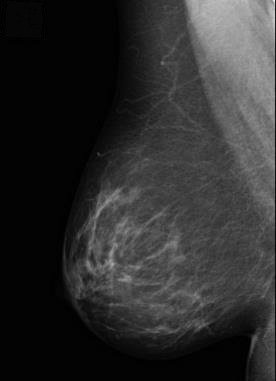
Category B
25-50% fibroglandular
(moderately dense tissue))
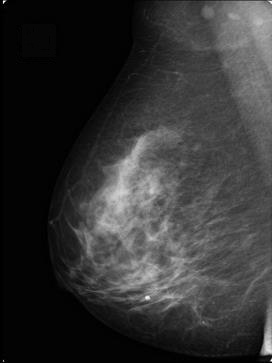
Category C
50-75% fibroglandular
(heterogeneously dense tissue)
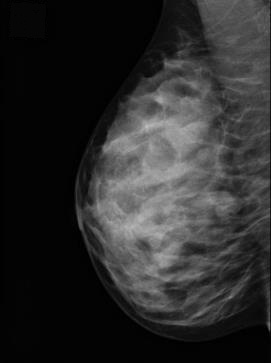
Category D
>75% fibroglandular
(extremely dense tissue with very little fat)
Research2 shows that a woman with extremely dense breast tissue has approximately five times greater risk of breast cancer than a woman with breast tissue density of <10%, all other factors being equal.
Increased mammographic density makes it more difficult to perceive a breast cancer on a mammogram
Both breast cancers and benign breast lesions (such as cysts and fibroadenomas), appear as white masses on a mammogram. They are therefore difficult to detect if the background breast tissue is also white (ie. fibroglandular) rather than fatty.
3D mammography (Digital Tomosynthesis) has approximately 25% better overall cancer detection rate than 2D (standard) mammography3
At Sydney Breast Clinic, we aim to optimise cancer detection by using the latest digital mammogram technology. Digital breast tomosynthesis, often called 3D mammography, is used for all women having a mammogram. DBT uses a series of angled images reconstructed into slices. This improves cancer detection (sensitivity) and confirms normal findings when superimposed normal breast tissue mimics an abnormality (specificity).
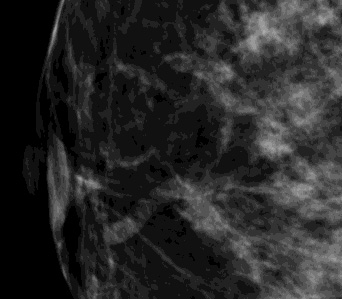
Figure 2. Standard mammogram
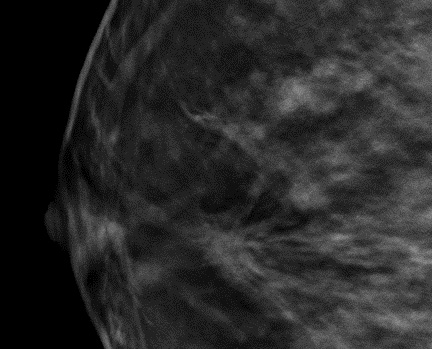
Figure 3. Tomogram of the same area
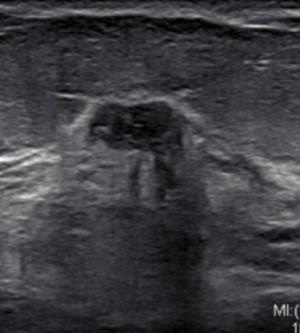
Figure 4. Ultrasound of the occult cancer
Ultrasound in addition to mammography will improve detection of asymptomatic cancer by up to 50%4
We use the mammographic density to guide the use of ultrasound examination. All women with category C or D mammographic density will be recommended a bilateral ultrasound examination following their mammogram and clinical examination, even if they are asymptomatic, and even if the tomogram showed no signs of malignancy. This is because we know that significant lesions may be obscured on mammography by general breast tissue density.
Recommended screening interval
At SBC the screening protocol is based on levels of risk and individually tailored: For asymptomatic women with no breast cancer risk factors at all (including tissue density), recommendations are:
- aged 40-49 years: screening mammogram annually
- aged 50-59 years: screening mammogram every 18 months
- aged 60 years and over: screening mammogram every 2 years
Asymptomatic women with significant breast cancer risk factors are advised to have annual screening with a mammogram and an ultrasound regardless of age. Breast MRI may also be indicated as an additional screening tool. Medicare-rebatable breast screening MRI is limited to particular situations and requires specialist referral to be rebated.
References:
- http://canceraustralia.gov.au/publications-and-resources/cancer-australia-publications/synoptic-breast-imaging-report-update
- Boyd NF, Guo H, Martin LJ, et al. Mammographic Density and the Risk and Detection of Breast Cancer. N Engl J Med 2007; 356:227-36
- Skaane P, Bandos AI, Guillen R, et al. Radiology 2013 Apr;267(1):47-56. doi: 10.1148/radiol.12121373. Epub 2013 Jan 7.
- Berg WA, Blume JD, Cormack JB, et al. JAMA 2008 May 14;299(18):2151-63. doi: 10.1001/jama.299.18.2151.
References:
- http://canceraustralia.gov.au/publications-and-resources/cancer-australia-publications/synoptic-breast-imaging-report-update
- Boyd NF, Guo H, Martin LJ, et al. Mammographic Density and the Risk and Detection of Breast Cancer. N Engl J Med 2007; 356:227-36
- Skaane P, Bandos AI, Guillen R, et al. Radiology 2013 Apr;267(1):47-56. doi: 10.1148/radiol.12121373. Epub 2013 Jan 7.
- Berg WA, Blume JD, Cormack JB, et al. JAMA 2008 May 14;299(18):2151-63. doi: 10.1001/jama.299.18.2151.








